RESEARCH
Numerical Simulation
Numerical simulation is a very useful tool in understanding the behaviour of biological tissue and the design of medical devices that interact mechanically with the human body. It can minimise the need for experimental testing and clinical validation when designing medical devices. However, to make numerical simulations representative of actual behaviour of biological tissue, or parts of the human body, accurate modelling of both tomography and material behaviour is needed. While the tomography of body organs, and its variation between individuals and with disease progression, is difficult to quantify, the main challenge is normally associated with the tissue’s material behaviour.
Group Studies
In the BioEG, significant effort has been made over many years to characterise the eye’s tomography and material behaviour as explained in different parts of this site.
A dedicated software package has been developed by the group to enable the creation of both idealised and patient-specific numerical models with ease and within seconds.
Numerical Simulation
Incorporate material and topographic characteristics

A. Ocular model meshing software
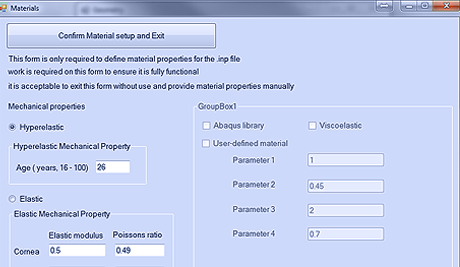
The complexity of ocular topography and the regional variation of thickness and material behaviour make the development of representative models of the human eye a non-trivial task. For this reason, significant effort has been made over 15 years by researchers of the OBG to build a dedicated software package that can create finite element models of the human eye.
The package can create both idealised and personalised models, the latter based on clinical topography and thickness data, and can consider the low stiffness of the epithelium and endothelium, the low shear stiffness of ocular tissue, the regional variation of stiffness across the globe and the specific features of the optic nerve head zone.
b. Numerical simulation of canine and human knee joints
Previous studies have shown that computational models of the stifle (knee) joint can be developed into powerful in silico tools for kinematic analysis of the joint, examining musculoskeletal mechanisms and injuries evaluating surgical procedures and designing artificial joints. In our studies, we have developed a FEM’s for canine stifle joints from high resolution Magnetic Resonance Imaging (MRI) data, focusing on the four major ligaments (cruciate and collateral), and the menisci and articular cartilages. Once validated, the FE models can be used in future studies to simulate joint stability when: (1) the extracellular matrix of the ligaments is manipulated, (2) the ligament is degenerated and injured.
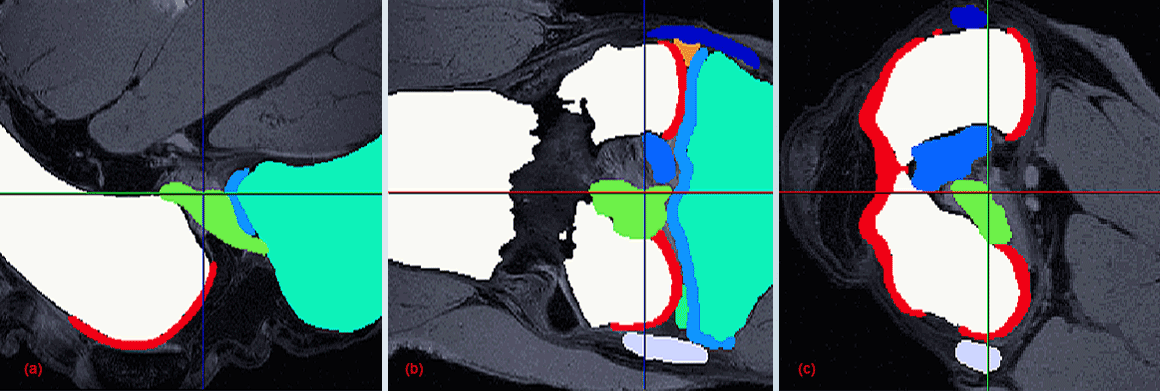
Segmented components of a stifle joint. Sagittal plane (a), coronal plane (b), and transverse plane (c).
c. Matching of corneal topography maps
The whole cornea cannot be reliably and accurately measured by a single videokeratography observation because of limitations in current topography instrumentation and measurement techniques.
Most VK instruments cover only the central cornea within an area of diameter that ranges between 8 and 10mm. To overcome this limitation and to obtain topography data that covers the entire corneal surface, a study has been done to match and combine topography maps taken for the central and peripheral cornea, producing a single map covering the whole corneal surface and extending beyond the edges of the limbus.
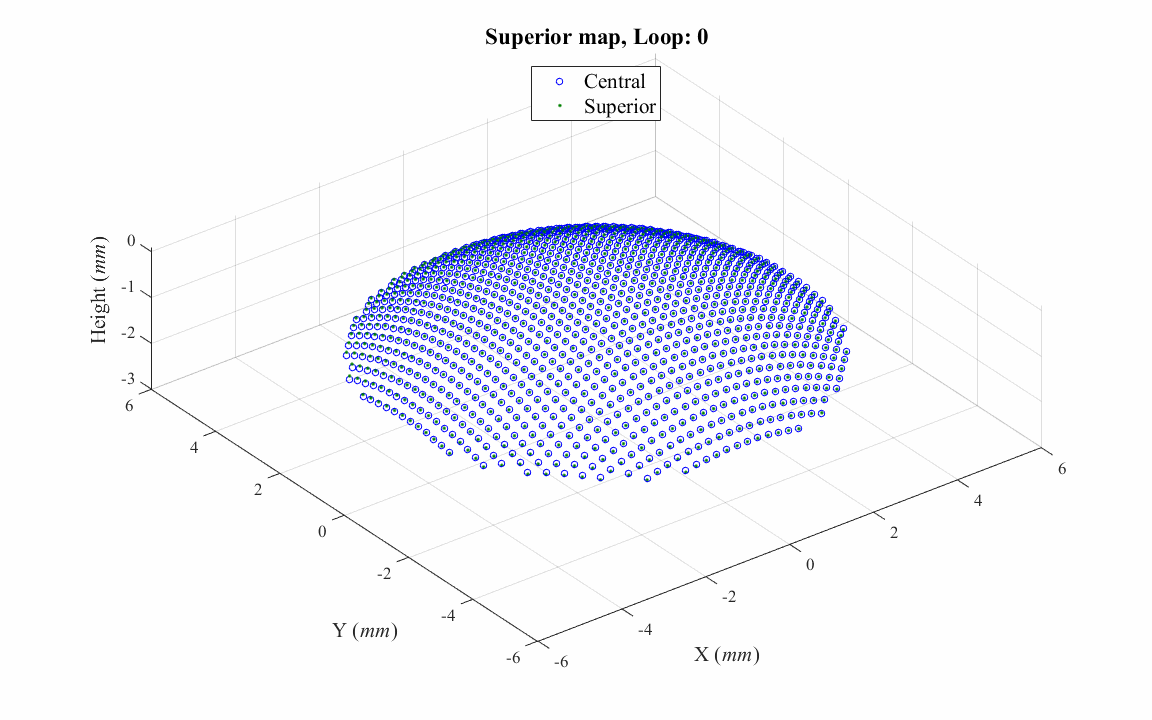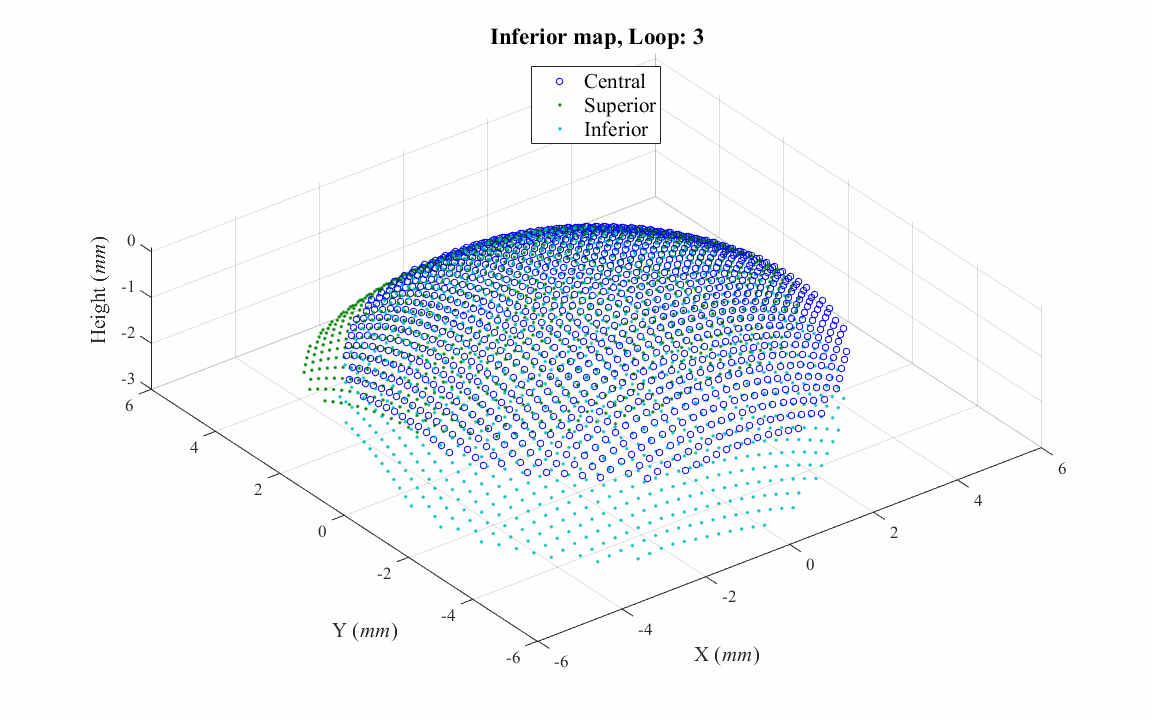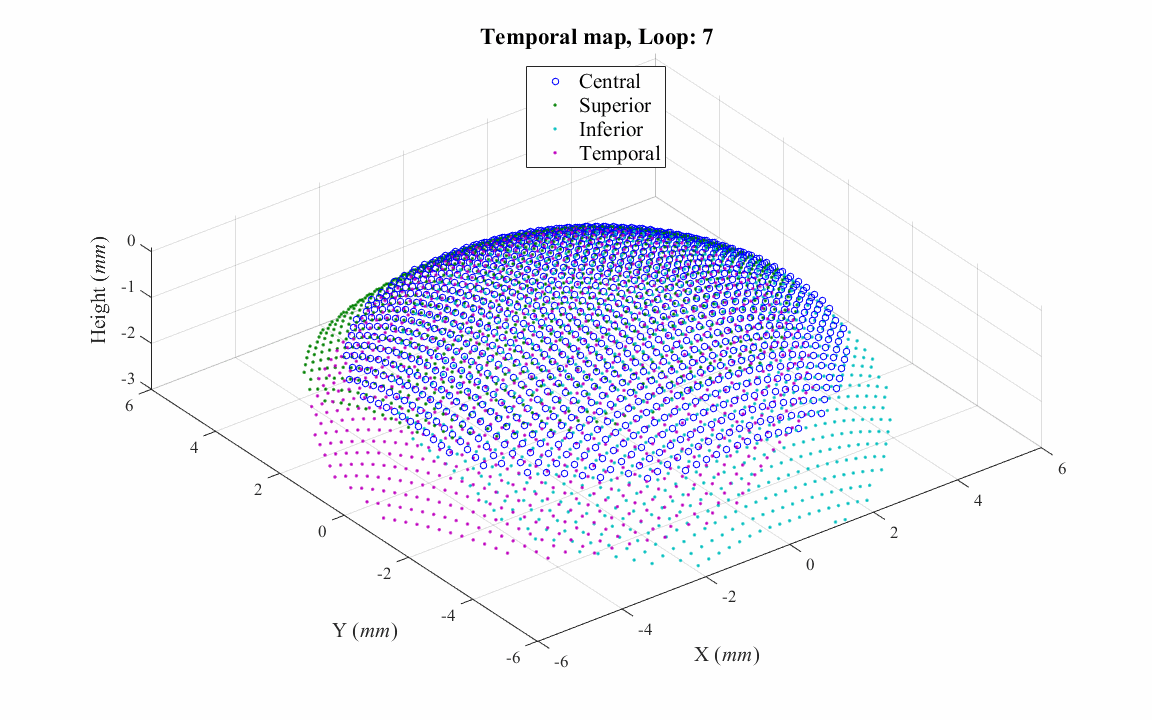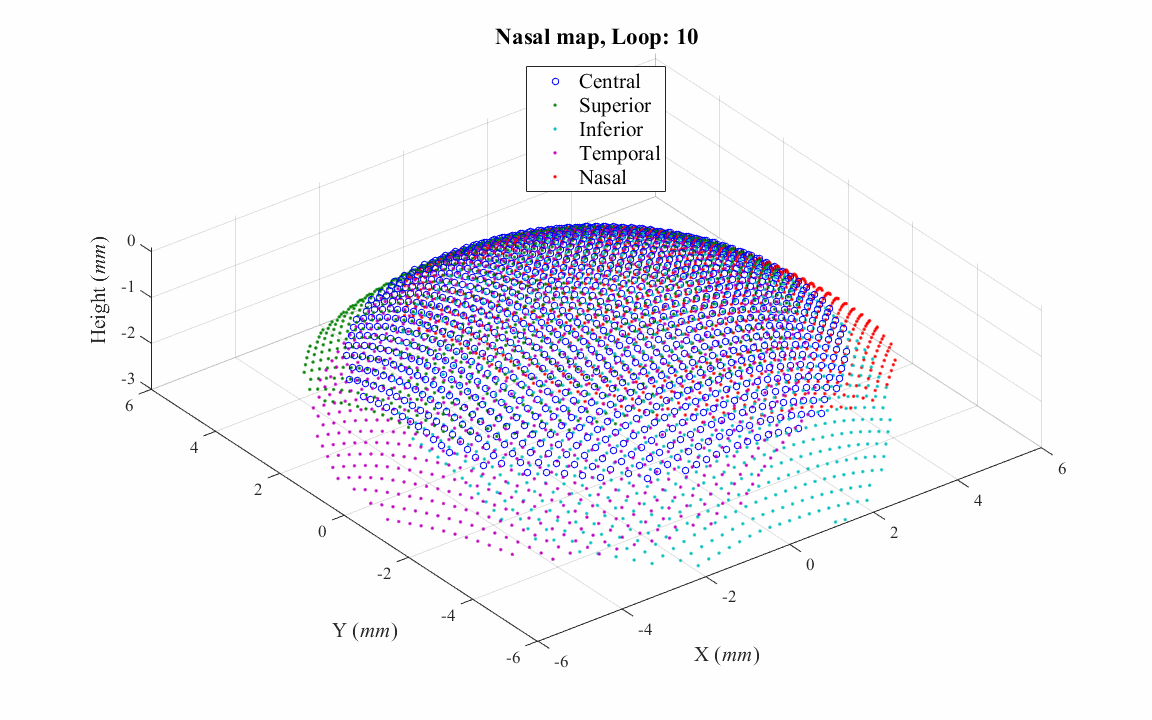
d. Correcting misalignment of topography maps
Repeated topography maps usually suffer from relative misalignment as patients are unlikely to be exactly in the same position and looking in the same direction while taking repeated measurements of their ocular topography. This misalignment leads to reduced confidence in the resulting maps, which are commonly used in diagnosis and management of a number of conditions that affect corneal topography such as keratoconus. The Group has carried out a study to use ICP algorithm to estimate and correct for misalignment between subsequent maps, resulting in significant improvements in data repeatability.

Distribution of elevation difference between successive corneal topographies before and after elimination of misalignment using ICP algorithm: Case 1. The first diagram shows contour maps of elevation difference in the common region of two successive anterior corneal topographies before (left) and after (right) elimination of misalignment using ICP algorithm, while the second diagram shows corresponding contour maps for posterior topographies. The four contour maps share the same colour scale (upright in µm). In this particular case, before ICP correction of misalignment, the RMS of fit error is 13.53 µm for both anterior and posterior surfaces, considered simultaneously, reduced to 7.24 µm (46.49% reduction) following the ICP correction.
e. Automated segmentation of optical coherence tomography scans
Optical coherence tomography (OCT) scans of the anterior segment cover all the cornea, limbus and part of the sclera. The scans, with their typical high resolution, offer the opportunity to provide sufficient topographic data to cover much more of the ocular globe than what could be obtained from videokeratography maps. The Group has carried out a study to use the graph method for the automatic segmentation of OCT 2D scans and then combine these segmentations to create accurate estimations of the 3D shape of the eye’s anterior segment, including both anterior and posterior surfaces. With this work, we now have the ability to build patient-specific, ocular numerical models that can be used for individual customisation of treatment.
f. Fluid Structure Interaction
The air puff test is a type of non-contact methods used in different areas to investigate the material behaviour or the biomechanical properties of biological tissues such as skin, cornea, and soft tissue tumours and also to study chicken embryogenesis, fruit firmness or meat tenderness. For the human eye, having a valid and complete numerical simulation of the air puff test is very helpful and can greatly benefit to reduce a lot of time and cost of experimental testing as it's considered as a benchmark test similar to tensile test to understand the behaviour of the cornea under different loading conditions. The gap in research in this area is considering the fluid structure interaction effect between the cornea, the air puff and the eye internal fluid. The simulation of the air puff test on the human eye is a Multiphysics problem which means; coupling between different numerical models and solvers with different governing equations and exchanging the data between them during the solution.
OUR MAIN RESEARCH AREAS:
The Group carried out extensive tests to determine the mechanical properties of soft tissues.
more infoOur simulations represent closely the mechanical properties of materials and the organ’s topography.
more infoWe are involved in the developed of a number of medical devices to improve clinical practice.
more infoMathematical algorithms have been developed to improve customisation of surgical procedures.
more info